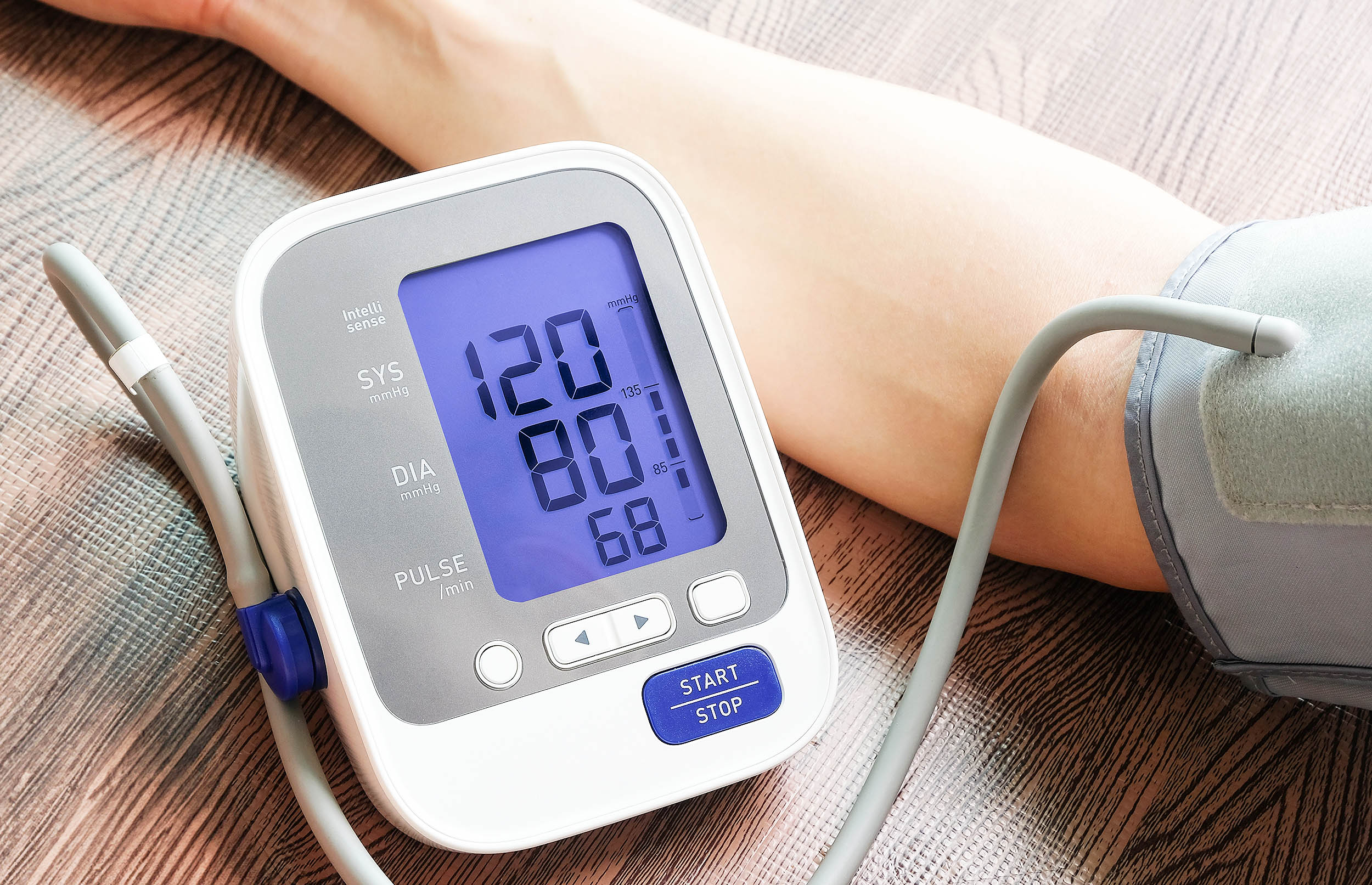
New Johns Hopkins Study Shows Arm Position Can Dramatically Skew Blood Pressure Readings
Johns Hopkins researchers confirm that subtle differences in arm positioning during blood pressure checks can inflate readings by up to 7 millimeters of mercury, potentially misleading millions of Americans living with or at risk for hypertension.
This urgent discovery reveals that letting the arm dangle unsupported rather than resting it on a desk or firm surface can artificially nudge blood pressure numbers dangerously higher—sometimes pushing patients from an “elevated” category into high-risk “stage 2” territory.
Why This Matters Now
Hypertension remains a leading cause of heart attacks and strokes nationwide. Doctors depend on quick snapshots in clinics to decide whether to start lifelong medications, but the reliability of these readings is now in question.
“A 6.5 mmHg increase just because the arm isn’t supported is clinically significant,” says Sherry Liu, M.H.S. This difference can change a systolic reading from 123, which is mild, to 130, which crosses into Stage 1 hypertension.
The impact is massive: Nearly half of U.S. adults have high blood pressure, making accurate measurements fundamental to effective diagnosis and treatment.
How the Study Was Conducted
Led by Dr. Tammy Brady at the Johns Hopkins University School of Medicine, the study enrolled 133 Baltimore volunteers aged 18 to 80. Participants underwent blood pressure testing after walking two minutes to mimic real clinic prep, followed by five minutes of seated rest with back and feet supported.
The researchers tested three common arm positions — desk-supported, lap resting, and side dangling — using automated cuffs to eliminate human error. The desk-supported position served as the standard baseline, with arm position changes revealing significant fluctuations:
- Lap-supported arm raised systolic readings by 3.9 mmHg on average
- Unsupported, dangling arm spiked systolic by 6.5 mmHg and diastolic by 4.4 mmHg
These differences persisted across ages, body weights, and hypertension diagnoses, confirming the universal nature of the effect.
The Science Behind the Shift
The culprit is hydrostatic pressure. When the arm rests at heart level on a firm surface, blood pressure readings are more accurate. Dropping the arm below heart level means the heart must work against gravity to push blood upward, exaggerating the measured pressure.
The American Heart Association recommends patients sit with their backs supported, feet flat, legs uncrossed, and the arm resting on a firm surface at mid-heart height.
However, fast-paced clinics often shortcut these steps, leading to systemic overestimations that subtly but significantly skew patient charts. Over time, these errors can lead to unnecessary prescriptions or missed treatment opportunities.
Real-World Implications and Next Steps
Millions self-monitor blood pressure at home, often at kitchen tables that are too low. Experts suggest practical fixes like using pillows to raise the elbow or placing cuffs on counters to align with heart height.
Additionally, cuff size plays a role: about 12% of Black Americans have larger arm circumferences needing wider cuffs, or else readings can spike by 5 to 10 mmHg.
Brady’s team is testing user prompts on devices reminding patients or clinicians to “Rest arm on table” and exploring wrist cuffs with built-in position sensors to reduce errors.
Public-health experts hope better standardization could prevent thousands of unnecessary medication starts each year, cutting side effects and healthcare costs without compromising cardiac safety.
For patients and providers in North Carolina and nationwide, this breakthrough underscores a simple yet critical step: check arm position carefully during blood pressure tests—it can change lives.
“Almost right can still mean wrong for blood pressure measurement,” emphasized Dr. Tammy Brady.
The full study appears in JAMA Internal Medicine, signaling a call to action for clinics and home monitors alike.