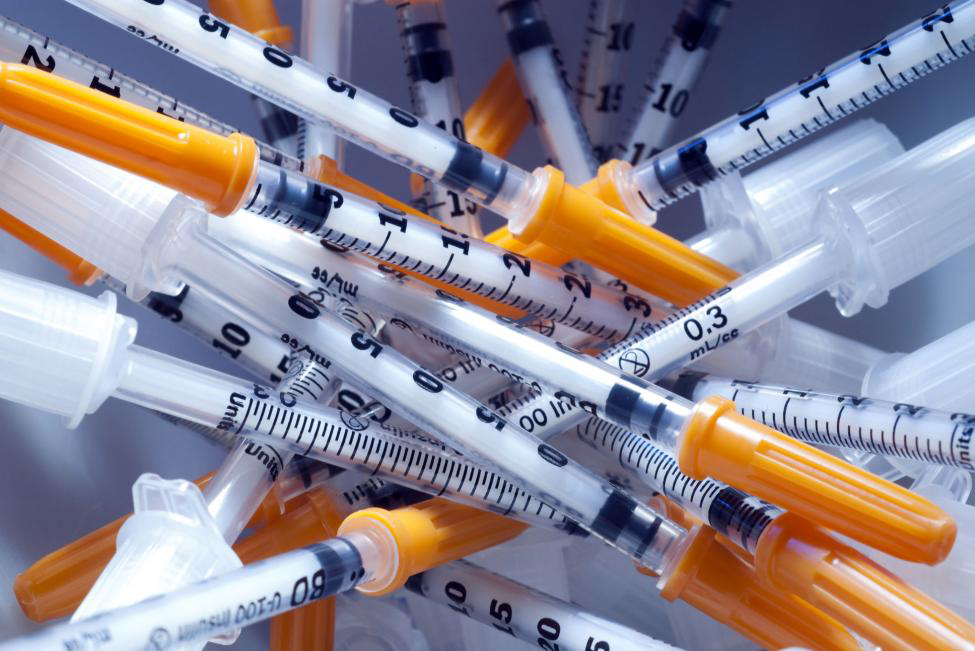
More Americans are increasingly turning to unapproved peptides, which are marketed as solutions for building muscle, enhancing skin, and prolonging life. This trend reflects a growing interest in alternative therapies and wellness practices. A significant driver of this movement is the rising popularity of GLP-1 weight loss medications, a class of approved peptides that help users achieve rapid weight loss. In contrast, the peptides being promoted by influencers and wellness advocates often lack approval for human use, with much of the supporting evidence derived from animal studies.
Some of these peptides, including BPC-157 and TB-500, are classified as banned substances by international sports authorities due to their doping potential. “None of them are proven,” stated Dr. Eric Topol, a renowned research methods expert and director of the Scripps Research Translational Institute. He emphasized that these substances have not undergone adequate clinical trials, yet many individuals are opting to use them. This phenomenon has sparked considerable concern among health professionals.
A notable figure supporting the use of peptides is Robert F. Kennedy Jr., the Health Secretary, who has garnered a significant following among Americans skeptical of traditional medicine and pharmaceutical companies. The Food and Drug Administration (FDA) has long attempted to regulate this market, issuing warning letters to clinics that promote such products. In March 2023, the FDA added over two dozen peptides to a list of substances that specialty pharmacies should not be compounding, indicating a stricter approach to regulation.
Kennedy has expressed his intention to challenge the FDA’s stance on these substances, advocating for the rights of individuals to access alternative treatments as part of his Make America Healthy Again movement. His support network includes figures like Gary Brecka, a self-proclaimed biohacker and longevity expert, who sells peptide injectables and patches through his website for prices ranging from $350 to $600 each.
Peptides, the building blocks of proteins, play crucial roles in the human body, triggering hormones necessary for growth, metabolism, and healing. While the FDA has approved certain peptides, such as insulin for diabetics and human growth hormone for children with developmental disorders, many others being marketed lack formal approval, making their sale technically illegal. Under current FDA guidelines, these unapproved peptides also cannot be compounded, which is the process where pharmacies create custom medications for patients.
Despite this, influencers like Joe Rogan have publicly endorsed specific peptides, such as BPC-157, claiming significant health benefits. Rogan shared his experience of overcoming elbow tendonitis in just two weeks after using this peptide. His endorsement has contributed to the rise of companies like Ways 2 Well, a Texas-based clinic offering various alternative treatments, including peptides. For $99, the clinic provides a consultation that includes shipping peptide vials along with necessary dosing instructions.
Many proponents argue that peptides serve as natural alternatives to conventional medicine. Andrea Steinbrenner, a consulting executive, shared her motivation for exploring peptides, citing their potential benefits for longevity and energy. She and her husband now receive monthly infusions at a clinic, supplementing their regimen with daily peptides.
Despite claims of safety due to their natural origins, critics warn that the peptides sold online are often synthetically produced and can carry significant health risks. Dr. Anita Gupta of Johns Hopkins School of Medicine emphasizes the importance of consulting healthcare professionals about the long-term safety of these products.
Concerns surrounding the marketing of peptides extend to the terminology used to navigate regulatory frameworks. Many companies utilize phrases like “research use only” to sidestep FDA oversight. This language is prevalent among online communities sharing tips on purchasing and using these substances. Legal experts note that this is a tactic to bypass regulations, as unapproved chemicals intended for human use fall outside FDA jurisdiction.
The FDA has made efforts to restrict the availability of peptides, particularly during the COVID-19 pandemic, when it issued numerous warning letters to businesses claiming that certain peptides could enhance immunity. The agency further solidified its position by adding nearly 20 peptides to its high-risk substances list, resulting in fines and legal actions against compounding pharmacies that violate these regulations.
This regulatory push has led to backlash from wellness advocates, including a lawsuit filed by a prominent compounding pharmacy claiming that the FDA neglected proper legal procedures when adding peptides to its restricted list. The litigation prompted the FDA to reconsider its stance and convene public meetings to assess the safety of several peptides flagged for risks. Experts at these meetings largely supported the FDA’s assessments, affirming the need for caution.
However, some industry voices argue that physicians should have access to all potential treatment options. Lee Rosebush, who was involved in the lawsuit against the FDA, asserts that the agency’s inaction limits medical professionals’ ability to provide comprehensive care.
Recent developments suggest that the FDA may be poised to alter its approach. The agency has recently removed several experts from its compounding advisory panel, potentially opening the door for the appointment of individuals more favorable to peptide therapies. This shift could lead to either a revised list of approved peptides or a more lenient stance on enforcement against their use.
As interest in peptides continues to grow, healthcare professionals are increasingly encountering patients eager to explore these therapies. Dr. Gupta urges individuals to prioritize safety and engage in open discussions with their healthcare providers about the implications of using unapproved peptides. “Patients should be really asking their health care professionals: Are these medications safe long term?” she advised.