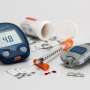
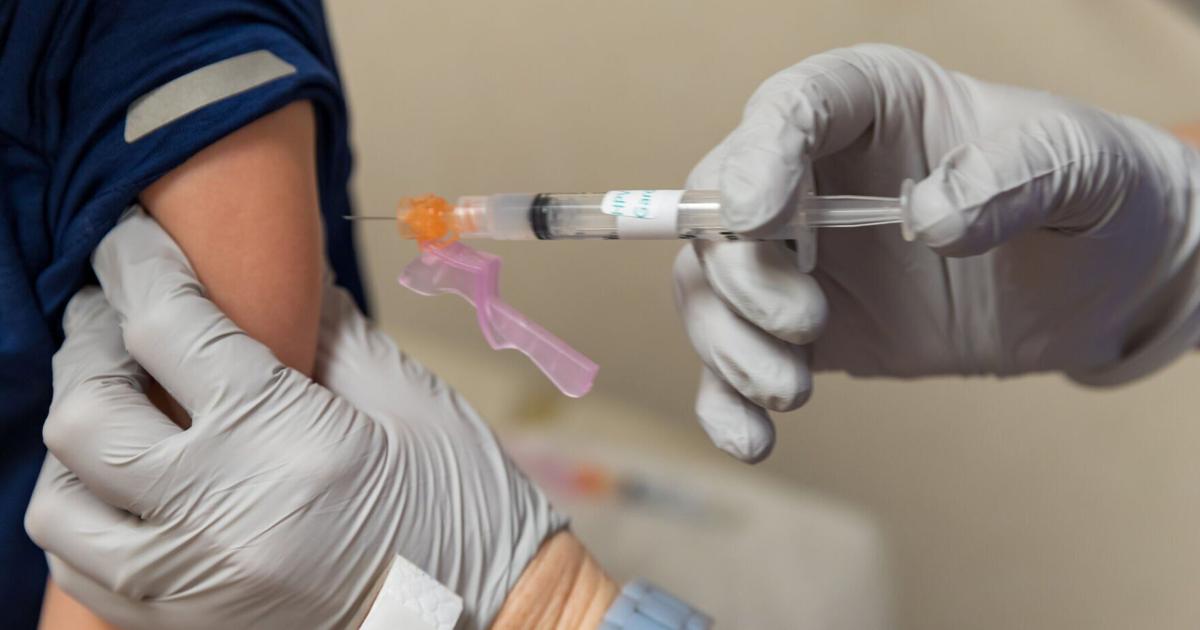
November is designated as National Diabetes Month, a time when discussions about diabetes prevention, management, and its impact become particularly prominent. Among the various forms of diabetes, type 1 diabetes stands out as a significant autoimmune condition, especially in children and adolescents. This chronic disease does not have a known cure and occurs when the body fails to produce sufficient amounts of insulin, a hormone essential for converting food into energy.
Type 1 diabetes, often referred to as juvenile diabetes, arises when the immune system mistakenly attacks and destroys the beta cells in the pancreas responsible for insulin production. Without adequate insulin, glucose remains in the bloodstream, leading to high blood sugar levels, known as hyperglycemia. This condition can have severe health implications, including the body resorting to breaking down fat for energy, which produces harmful acidic compounds called ketones.
Symptoms associated with type 1 diabetes primarily stem from the body’s inability to utilize glucose effectively. Common indicators in children include increased thirst, frequent urination, and extreme hunger, often accompanied by weight loss. Other symptoms may include irritability and blurry vision, particularly when blood sugar levels are dangerously high. If not treated promptly, type 1 diabetes can escalate into a medical emergency characterized by symptoms such as nausea, vomiting, rapid breathing, and loss of consciousness.
Diagnosis of type 1 diabetes typically occurs when a child exhibits classic symptoms alongside elevated blood sugar levels. Medical professionals may utilize the hemoglobin A1c (HbA1c) test, which assesses average blood sugar levels over the past three months, or an oral glucose tolerance test (OGTT). In some cases, testing for ketones in urine can also provide critical diagnostic information. Factors such as age and the presence of specific proteins called islet autoantibodies can help distinguish between type 1 and type 2 diabetes.
Treatment for type 1 diabetes focuses on normalizing blood sugar levels, a task that requires continuous monitoring. Patients often utilize a blood glucose meter for regular checks or a continuous glucose monitor (CGM), which provides real-time glucose readings. Insulin therapy, administered via daily injections or an insulin pump, is essential for managing the condition. Injections typically occur in areas of fatty tissue, including the abdomen and thighs, while insulin pumps deliver insulin through a cannula placed under the skin.
Diet plays a crucial role in managing type 1 diabetes. Insulin doses must correspond with carbohydrate intake, and physical activity can necessitate adjustments in insulin levels. Some insulin pumps have features designed to reduce insulin delivery during exercise or sleep, thereby minimizing the risk of hypoglycemia, or low blood sugar.
Advancements in technology have led to the development of automated insulin delivery systems (AID), which enhance diabetes management by enabling communication between insulin pumps and CGMs. These systems can automatically adjust insulin delivery based on real-time glucose readings, helping to maintain stable blood sugar levels.
Research continues to explore the possibility of early detection of type 1 diabetes, particularly for individuals at higher risk, such as those with a family history of the disease. Screening programs may identify potential cases before symptoms manifest. While type 1 diabetes cannot currently be prevented, new medications are available that may delay its onset in certain high-risk individuals, targeting the immune cells that attack insulin-producing cells within the pancreas.
The journey of managing type 1 diabetes is ongoing, with innovations in treatment and monitoring providing hope for improved quality of life for those affected. Awareness efforts during National Diabetes Month aim to educate the public on the challenges and management strategies associated with this prevalent condition.